What are Dental Implants?
A dental implant is a titanium post (like a tooth root) that is surgically positioned into the jawbone beneath the gum line that allows your dentist to mount replacement teeth or a bridge into that area. It is a safe and proven effective replacement for the tooth root – the very foundation of a natural tooth. It provides a strong foundation for fixed (permanent) or removable replacement teeth that are made to match the natural teeth. 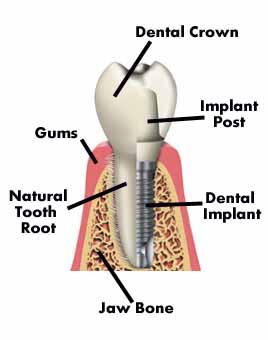
Get in Touch with Medical Experts
They are made of titanium, (a biocompatible material that is accepted by the body and serves as a strong and sturdy foundation for replacement teeth). This metal has a unique ability to fuse directly to bone through a process known as osseointegration (“Osseo” – bone; “integration” – fusion with). It is extremely important, then, for the implant to be engineered in a way that will maximize its surface area-to-bone contact.
A dental implant is a good option for people who have lost a tooth or teeth due to periodontal disease, an injury, or some other reason.
Who Should Get Dental Implant?
The ideal candidate for a dental implant should be in good general and oral health.
For going for a dental implant you should meet the following basic criteria:
-
Have healthy teeth and gums
-
Have sufficient bone density to support the dental implant
-
Are committed to good oral hygiene
-
Have not had treatment with bisphosphonate medications (usually for cancer treatment)
-
Are non-smokers or are willing to stop smoking during the dental implant process
-
Understand that the process can take four to twelve months, and are willing to commit this amount of time to the dental implant procedure
-
After the bone material is placed, it can take a full six months to heal. The implant is placed after the bone grafting site has healed. After the implant is placed it can take an additional six months to heal before the crown can be placed.
Some people may not be good candidates for implants. They include:
-
Young people whose jawbones have not stopped growing
-
Heavy smokers — Smoking hinders healing in the mouth. It can reduce the likelihood of a successful implant.
-
Alcohol or substance abusers who are not prepared to follow the dentist's instructions after placement of the implant, such as no smoking, and returning for follow-up. They also may be less likely to take good care of their teeth and gums.
-
People who have received high-dose radiation treatment of the head or neck
-
People with chronic diseases or systemic problems, including:
-
Uncontrolled diabetes
-
Connective-tissue diseases
-
Hemophilia
-
Significant immune deficiencies
-
-
People who take certain medicines, such as steroids or drugs that suppress the immune system
-
People who severely grind or clench their teeth — These habits can place too much pressure on the implants and increase the risk of failure
-
Pregnant women
You still may be a good candidate for implants even if you have one of these conditions. It depends on the extent and severity of the condition. Your dentist can evaluate you to see if you would be a good candidate for implants.
Know More:
Types of Dental Implants
There are three types of implants, and they can be described according to their shape, placement or by the procedure used to attach them to the jaw (single or two-stage).
ENDOSSEOUS -“within the bone”
These are commonly used for the two-stage procedure. They are surgically implanted directly into the jaw bone. Once the surrounding gum tissue has healed, a second surgery is needed to connect a post to the original implant. Finally, an artificial tooth (or teeth) is attached to the post-individually or grouped on a bridge or denture

Each implant holds one or more prosthetic teeth. This type of implant is generally used as an alternative for patients with bridges or removable dentures.
They are usually shaped like a screw or cylinder and are made either of metal, metal covered with ceramic, or ceramic material.
SUBPERIOSTEAL -“on top of the bone”
These are commonly used for single stage procedures. These consist of a metal frame that is fitted just below the gum tissue on the jaw bone. As the gums heal, the frame becomes fixed to the jawbone. Post, which is attached to the frame, protrudes from the gums to hold the restoration.
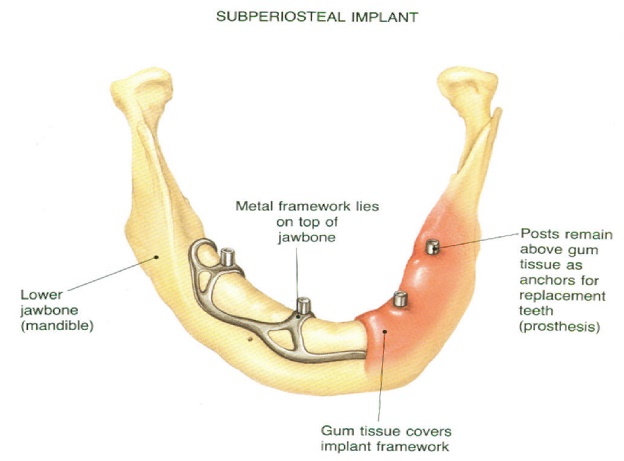
The primary advantage of this type of implant is that it can hold dentures securely for individuals who do not have enough bone height.
Advantages of Dental Implants
There are many advantages to dental implants, including:
-
Next best thing to healthy, natural teeth: Strong and stable, a dental implant restores a lost tooth so that it looks, feels, fits and functions like a natural tooth. And because they are designed to fuse with bone, they become permanent.
-
Speakeasy: With poor-fitting dentures, the teeth can slip within the mouth causing you to mumble or slur your words. Dental implants allow you to speak without the worry that teeth might slip.
-
Improved comfort. Because they become part of you, implants eliminate the discomfort of removable dentures.
-
Eat your favorite food: Sliding dentures can make chewing difficult. Dental implants function like your own teeth, allowing you to eat your favorite foods with confidence and without pain.
-
Retain your natural face shape, and smile: A face without teeth can sag and appear sunken and sad. Dental implants can give you back your smile and help you feel better about yourself.
-
Improved oral health. Dental implants don't require reducing other teeth, as a tooth-supported bridge does. Because nearby teeth are not altered to support the implant, more of your own teeth are left intact, improving long-term oral health. Individual implants also allow easier access between teeth, improving oral hygiene.
-
Built to last. Dental implants are a long-term solution: Implants are very durable and will last many years. With proper placement and good care, they may last a lifetime.
-
Convenience. Dental implants eliminate the embarrassing inconvenience of removing dentures, as well as the need for messy adhesives to keep them in place.
-
Protect your healthy bone: Leaving empty spaces in your mouth after losing one or more teeth can lead to additional health issues, such as the loss and deterioration of some of your jawbone. When it is not being used to support a natural tooth, the jawbone deteriorates, losing its strength and firmness. Dental implants are the only dental restoration option that preserves and stimulates the natural bone, actually helping to stimulate bone growth and prevent bone loss.
Dental Implants Procedure
The first step in the dental implant process is the development of an individualized treatment plan. The plan addresses your specific needs and is prepared by a team of professionals who are specially trained and experienced in oral surgery and restorative dentistry. This team approach provides coordinated care based on the implant option that is best for you.
Most dental implant surgery procedures are performed in the dentist's office and occasionally in a hospital setting. Local anesthesia (numbing of the area with small shots), is usually adequate for these out-patient procedures but various other forms of patient sedation (such as nitrous oxide, and oral/or intravenous sedation) may also be used. Adjunctive surgical procedures, such as bone augmentation, may be performed as separate procedures or at the same time as implant placement.
Each surgical procedure is different depending on the clinical situation as well as the preferences of the patient and dental practitioner/ surgeon.
Phase 1: Evaluation & preparation
Implant placement surgery is actually a relatively minor procedure, especially if appropriate pre-planning has been done ahead of time. This generally takes the form of
-
radiographic (x-ray) examination,
-
frequently CT scanning,
-
Often the use of a precision surgical guide.
This allows a determination of your occlusion (bite), where the new replacement teeth will be placed within it, exactly where the implants will be placed in the bone to support the teeth, and the bone quantity and quality into which they will be inserted.
Phase 2: Surgery (Implant placement)
One of the most important parts of the surgical procedure is what is referred to as “site preparation.” A relatively small channel, a hole, is prepared in the bone. This is referred to as an osteotomy (“osteo” – bone; “otomy” – to cut or separate). Small incisions into the gum tissue are used to access the bone thereby creating small “flaps” as they are called (like flaps on an envelope), to allow visualization of the bone's shape and location.
If a surgical template or guide has been made, it will be placed in the mouth, and the osteotomy sites prepared through it to ensure accurate positioning of the implants. A drilling sequence is used that progressively increases the size of the site until it mirrors the implant shape exactly to ensure the necessary precision fit. The drilling procedure is critical to implant success.
| Pre | Post |
 | 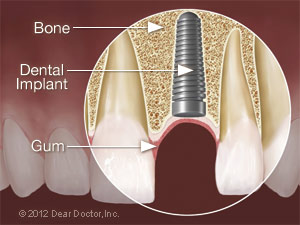 |
The next step is to place the implants straight into the sites so that the healing process can begin. Healing takes 3-6 months. Dental implants are sterile and it is critically important that their surfaces are untouched. The implants go from their sterile packaging into the osteotomy sites. Radiographs (x-ray pictures) are generally taken during or after the procedure to verify correct implant positioning.
The surgical procedure ends with the closure of the gum flap tissues. Often, sutures (stitches) are used that are self-absorbing and therefore do not need to be removed.
A period of several months after placement of the implant .will be required for it to fuse itself to the jawbone. A temporary crown can be placed over it during this period. The process of fusion is referred to as Osseointegration and is ultimately what will make your dental implant a permanent fixture of your mouth, similar to your natural teeth.
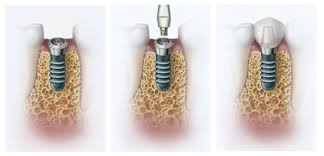
Phase 3: Placement of Crown
Once the dentist has determined that the titanium implant has properly fused to the jawbone, a dental crown – custom-designed to blend in with your natural teeth – will be affixed to the top of the implant.
An impression is made of your mouth and your new tooth or teeth are created so that they are the correct size, shape, and color for your mouth. This phase generally takes 2 visits about two weeks apart.
Post-surgery
Because of the nature of the surgery, and with the gentle tissue management described above, discomfort is minimal and healing is very predictable (95 - 97% success rates). However, every situation is different and your dentist will give you an insight as to what to expect in your situation.
The mild non-steroidal anti-inflammatory medication of the aspirin or ibuprofen family is usually all that is necessary to relieve any discomfort and swelling in the first two or three days. Antibiotics may also be prescribed to ensure healing, in addition to anti-bacterial mouth rinses, during the time that the gum tissues heal.
Risk of Dental Implants
As with any other surgical procedure, there are a variety of internal and external factors that cause complications or even total failure of the treatment. Dental Implants are no exception.
-
Peri-implantitis (Infection): Peri-implantitis, or infection, can set in when bacteria is present during oral surgery or any time post-surgery without proper dental hygiene.
-
Nerve & Tissue Damage: Another possible but rare problem is damage to the tissue surrounding the implant, specifically the nerves. When an implant is placed too close to a nerve, patients may experience chronic pain, tingling or numbness in their cheek, gums, tongue, lips or chin. The nerve damage could be temporary or permanent and the implant might need to be removed.
-
Failed Osseointegration (Implant is Loose or Fell Out): An implant is deemed a failure if it is mobile, falls out or shows signs of bone loss of more than 1 mm after the first year and more than 0.2 mm after the second year. Several factors can cause this to happen including incorrect positioning, insufficient bone density or volume, overloading, damage to surrounding tissues, external force/sudden impact, fractured implants or even a reaction to anesthesia
-
Sinus Problems: Sinuses can be a major challenge for dental implants replacing teeth in the upper row. In addition to the presence of the sinuses, insufficient bone quality and quantity in the upper back jaw can make dental implant procedures in this area difficult.
-
Other Risks & Causes of Failure: The following are other risks and causes of dental implant challenges for patients to consider.
-
-
Foreign body rejection
-
Failure of the implant itself
-
Allergic reaction
-
Dental Implant Success rate
The success of dental implants depends on both the patient and the dental surgeon.
Success rates of dental implants vary, depending on where in the jaw the implants are placed but, in general, dental implants have a success rate of up to 98%. With proper care, implants can last a lifetime.
Majority of the problems that do occur are minor and easily resolved. If something does go wrong, consult your dentist or surgeon as soon as possible. Fast response enables them to take corrective actions before you or the implant is threatened by additional (more serious) problems, which is why it’s important to be aware of the possible complications.
Maintenance of Dental Implants
Good oral hygiene must take place before, during, and after placement of dental implants to ensure the health of the implant.
Taking good care of your dental implants is vital for long-term success. With proper home care and professional maintenance, your new teeth can last for life.
The daily care of dental implants is very similar to the care of natural teeth. Restored dental implants should be kept clean and plaque free twice a day using a brush and floss. Cleaning is especially important after meals. This is accomplished by gently brushing, giving special attention to all sides of the implant.
-
A small, soft, manual toothbrush or an electric brush
-
Low-abrasive, tartar-control toothpaste
-
Dental floss for cleaning around the abutments
-
Antimicrobial mouth rinses
-
Inter-dental brushes or other aids for removing plaque between the teeth on either side of the implant(s)
-
Avoid damaging habits: teeth. Don't chew hard items, such as ice and hard candy, which can break your crowns — or your natural teeth. Avoid tooth-staining tobacco and caffeine products. Get treatment if you grind you
-
See your dentist regularly: It is recommended that you see your dentist every 3-6 months for a professional exam and cleaning. The implant(s) should be examined with an x-ray annually.
FAQ’s
Q. Why would I need a dental implant?
-
If you lose a tooth as a result of an accident, tooth decay, root canal failure, or gum disease, your dentist may recommend a dental implant and an artificial replacement tooth (a crown or cap). Dental implants also may serve as secure anchors for a bridge or dentures if you have multiple missing teeth.
Q. What is the minimum age for dental implants?
-
Dental implants can be placed any time after adolescence or when bone growth is complete.
Q. Why should I get a dental implant rather than just dentures or a bridge?
-
Dental implants are stronger and more durable than dentures or a bridge. They offer a permanent solution to tooth loss. In the case of multiple missing teeth, dental implants may be used to support a dental bridge or with dentures to increase stability and reduce gum irritation.
Q. What can happen if I don’t replace a missing tooth?
-
When you don’t replace a missing tooth, it can result in damage to adjacent teeth by causing gum recession and bone loss around those teeth. It can cause your other teeth to wear prematurely. You may experience difficulty eating and speaking, shifting teeth, jaw aches, and headaches.
-
Also, when you lose a tooth and its accompanying root, you can experience bone loss in your jaw. A dental implant gives the bone purpose, providing it with something to hold onto.
-
If a great deal of time has passed since the tooth came out and too much bone in the jaw has been lost, grafting may be necessary to increase bone mass before an implant procedure can be done
Q. Is the dental implant procedure painful?
-
A combination of local anesthesia and sedation dentistry, if necessary, is used during implant placement, so patients do not feel pain during the procedure. After the initial surgery, discomfort should be minimal. However, prescription pain medications may be prescribed to relieve any post-surgical pain or discomfort.
-
If you have any anxiety about the surgery, tell your dentist ahead of time. Mild apprehension can be relieved with sedative or anti-anxiety pre-medication given either orally or intravenously.
Q. What kind of anesthesia will I have?
-
In many cases, the entire implant procedure can be performed using local anesthesia.
Q. How long does dental implant surgery take?
-
Surgery time varies according to the number of implants you need. One implant usually will take just over an hour. Multiple implants generally take no more than two or three hours.
Q. What happens after my dental implant has healed?
-
After osseointegration has occurred (this can take up to six months), your dentist will remove the protective cover and place a healing abutment on top of the dental implant. Once the gum has grown around the healing abutment, your dentist will replace the healing abutment with a permanent crown.
-
If you have been wearing a temporary crown on the healing implant, after three to six months your dentist will change the temporary crown to a permanent crown
Q. When will I receive my new teeth?
-
Treatment time varies by patient. Typically, you will have some type of temporary teeth until your implants integrate with the bone. Your clinician can provide a time estimate based on your treatment needs.
Q. What if I want "metal-free" implants?
-
Firstly, there is no such thing as “metal-free” teeth. Almost all materials used for teeth replacements have some sort of metal ions in them. Dental implants are made of titanium alloy (similar to hip implants, shoulder implants, and knee implants), which is highly biocompatible, and allergy to titanium is extremely rare!
-
Currently, there are no proven alternatives to titanium dental implants.
Q. Can smokers have dental implants?
-
Dentists strongly advise patients to quit smoking before undergoing a dental implant procedure. Smokers are at higher risk for dental implant failure.
Q. What is all on four?
-
All on 4 is a trademarked treatment procedure that essentially involves the replacement of all missing teeth in one jaw by using only 4 implants. This procedure is especially beneficial in patients who have lost a lot of bone in the back areas of the mouth.
Q. Can dentures be made into implants?
-
Dentures cannot be “made into implants.” Implants are metal screws placed into the jawbone to help anchor and support artificial teeth (dentures). It may be possible to have implants placed beneath existing dentures to aid in the stabilization and support for those dentures. This could only be done if the current dentures were otherwise in excellent condition.
Q. How do dental implants help if I have full dentures or partial dentures?
-
Actually, implants are most popularly used in patients who wear full dentures or partial dentures. Dental implants can be used to provide retention and support for a removable implant overdenture, which basically snaps on the implants like a trailer-hitch! Therefore the partial or full denture does not move and reduces the dependency on denture adhesives/denture glue.
Q. Are dental implants safe?
-
Dental implants are a safe and clinically proven alternative to bridges and dentures for replacing missing teeth in qualified candidates.
-
People with certain risk factors, such as smokers, and those with inadequate bone density or who are immune-compromised, may not qualify for implant treatment.
Q. Do dental implants work?
-
Dental implants are among the most predictable tooth replacement options.
-
While there is no guarantee that an implant procedure will be successful, studies have shown a five-year success rate of 95 percent for lower jaw implants and a 90 percent success rate for upper jaw implants.
Q. How soon may I return to work after treatment?
-
You may return to work the next day unless otherwise instructed by your clinician. You may be prescribed medication to alleviate any minor discomfort you may have.
Q. How does the long-term value of implants compare to other treatment options?
-
Dental implants are low maintenance and provide stability and confidence in your smile. Therefore, the long-term value of dental implants far exceeds conventional treatment options.
Q. Are dental implants covered by insurance?
-
Coverage of dental implant treatment is determined by individual insurance companies. The number of dental insurance companies may pay toward treatment varies.